Gas Stations in Texas
This is a photo that I recently took outside of a gas station between Houston and Austin:

Now, if you haven’t been to a Buc-ee’s (pronounced “Bucky’s”), it is more like the size of a small grocery store than a regular gas station. There are dozens if not a hundred gas pumps, fresh barbequed brisket, a clothing section, a drink station with 30-40 kinds of soft drinks (many of them obscure), and more. It’s huge, and it’s a very popular Texas road stop for the quality of the food and snacks, the amenities, etc.

Look at the starting salaries for assistant managers: $100k+ a year on up. In fact, here’s a job ad for a Buc-ee’s in Florida paying $125k for the assistant manager position.
Job requirements? Just have a college degree (from anywhere, in any subject) and 1-2 years’ experience.

Indeed, if you work your way up to General Manager at this chain of gas stations, you could easily earn more than the NIH Director (!), and you wouldn’t even have to divest from anything.
***
Let’s imagine that the United States government started subsidizing the training of Buc-ee’s managers, e.g., by paying people a low wage to spend several years in training so as to be better prepared to enter the privileged ranks of Assistant General Managers who earn $100k or more a year.
[This isn’t as ludicrous as it sounds: The US government sponsors many job training programs through the Department of Labor, and states typically do likewise.]
But suppose that after several years, it turned out that many more people entered the official US/Buc-ee’s training program than could ever get jobs as a manager at Buc-ee’s. And suppose that many of them stayed in the program for 5, 6, 7, even 8 years in the hopes of finally getting a Buc-ee’s job that would never materialize. And suppose that it turned out that they were actually doing a lot of free work for Buc-ee’s in the meantime — even including work that the Assistant General Managers were supposedly paid to do.
At some point, it would be reasonable to ask:
- Is it fair to all these people to let them spend so many years in training programs for jobs they won’t get?
- Why are we subsidizing them to do so?
- Wait, hold up, we are subsidizing free workers for Buc-ee’s?
NIH and Post-Docs
An NIH working group on post-docs recently recommended that the minimum salary for post-docs be set at $70,000, a significant raise from the current minimum salary of $56,484. The advisory committee also recommended limiting the number of post-doc years to a mere five. See the full report here.
The working group was motivated by very real concerns about the academic biomedical workforce. Consider that in 2021, only around 27% of people with biomedical doctorates tried to go into academia, compared to 54% going into industry.
This isn’t surprising: As the report noted, “While the NIH NRSA stipend has been steadily growing and is $56,484 for a first-year postdoctoral fellow in FY 2023, it has not kept pace with inflation and is much lower than corresponding industry salaries.” Or consider the subhead on a Nature editorial from October: “Postdoctoral dissatisfaction about pay, job security, and career progression cannot continue. Institutions must up their game or risk losing the next generation.”

In other words, if biomedical academia is so uncompetitive compared to industry, that will have serious implications for:
- who is left to conduct basic research unconfined by industry’s demand for a marketable result, and
- who will end up training the next generation of scientists.
It’s a real worry.
The proposed NIH policy is a significant step in the right direction, both when it comes to pay and other issues (such as the need for NIH to work with NSF and/or the Institute for Research on Innovation & Science (IRIS) at the University of Michigan on getting better information about post-doc status).
That is all good, and I applaud my colleagues who were involved in this effort.
HOWEVER . . .
Even if the NIH adopts the working group’s recommendations, the following will still be the typical path for entering biomedical academia:
Do an undergraduate degree, then spend the next 6-8 years doing a PhD in biomedical sciences.
By the time you’re around 30 — perhaps the peak time for when many people might want to start a family — it’s time to spend up to several years doing post-docs where you are mostly providing labor for someone else’s scientific research, at a salary that might be 70% of what you could have earned at a large gas station (with no PhD).
Then, if you’re really lucky, you might get your first major NIH grant by the tender age of 36.
But if you’re the median researcher who makes it in academia at all, you’ll probably be 41 years old by the time you get that first grant (and there’s a 50% chance you’ll be over 41).
If you’re lucky enough to be on the tenure track, you’ll hopefully find out about tenure by the time you’re mid-to-late 40s — a perfect time to worry about having to uproot or change careers, eh?
In other words, biomedical academia has managed to create a career track that doesn’t fit well with how most people want to live their lives, or even with scientific progress (think of how many major discoveries have been made by people in their 20s—Newton, Einstein, etc.).
Fair Pay for Post-Docs
We need to pay post-docs a fair wage for their time and skills, and make it more appetizing (or even possible) for more good scientists to stay in academia. What would this look like?
Consider a few basic principles:
First, a popular guideline is that you shouldn’t spend more than 30% of your income on rent. Given the housing market recently, let’s raise that to 40%.
Second, a modest suggestion is that post-docs should be able to rent a one-bedroom apartment (if not more) within a 30-minute commute of their university.
Conclusion: a post-doc salary should be at least 2.5 times the median one-bedroom apartment rent within a 30-minute commute of their university.
What would this look like in practice? Consider Stanford. According to Apartments.com, the median one-bedroom apartment available within 30 minutes of Stanford is around $3,200 a month (at the time of my search). [Even at a Stanford-owned apartment complex where post-docs have priority, a one-bedroom apartment ranges from $2,345 (for the smallest one-bedroom) to up to $3,340 for a luxurious 1,040 square feet.]
By my modest standard, then, postdocs at Stanford should be paid at least $96,000 a year.
That sounds extravagant, of course, compared to current standards. But at least one Stanford professor would agree:
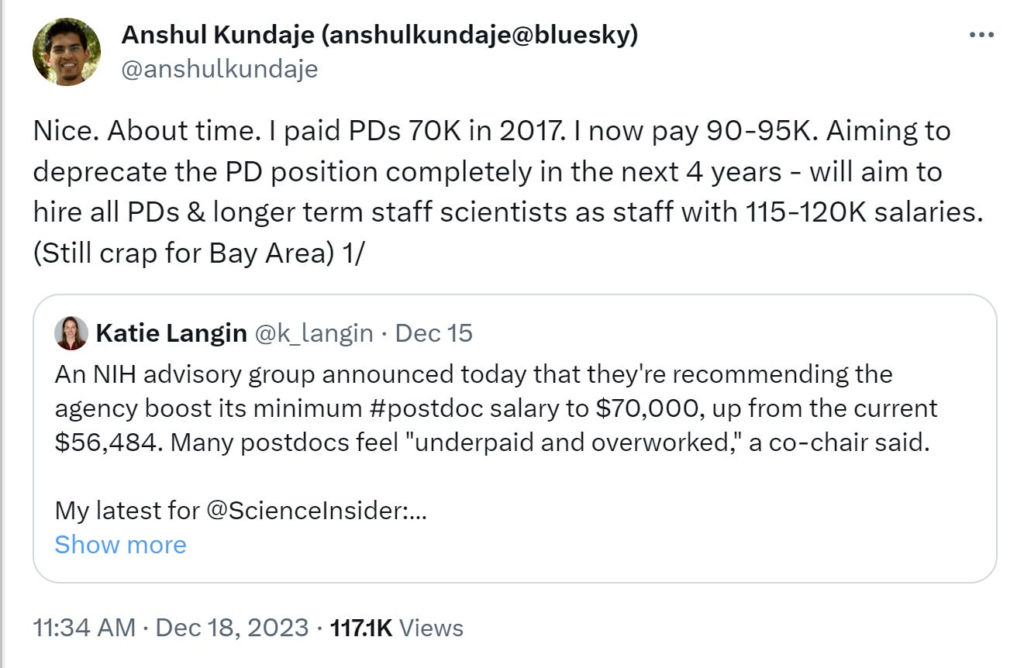
People who are mostly in their 30s and who are highly-trained PhDs deserve to have at least a one-bedroom apartment (which they could then supplement with a roommate or spouse).
If they don’t deserve a one-bedroom apartment, then what? Should they have to live 1-2 hours away? Sleep in a bunk bed with 4 roommates? Live in a tent under a bridge? Who will enter biomedical academia if they have to spend a large part of their 30s unable to afford even a tiny one-bedroom apartment without external help from generous parents or a beleaguered spouse?
Subsidizing Demand Isn’t a Good Idea
We shouldn’t pay for so many people to try to enter biomedical academia. Alternatively, we could ramp up spending while holding the number of subsidized graduate students and post-docs constant, so as to achieve better balance in the future. But either way, we have to stop subsidizing a disproportionately high number of biomedical trainees.
One of the worst ideas across many areas of public policy is to artificially subsidize the demand for some good (e.g., housing, healthcare, or biomedical professorships), while the supply is limited. That just creates wasteful and inefficient hypercompetition for the few slots available.
It’s like paying 50 people to spend several years prepping to be a Buc-ee’s assistant manager when there are only 10 positions available.
That’s what we’ve been doing in biomedical academia. Via NIH grants, we subsidize the production of graduate students and post-docs far beyond the number of academic positions that are available and that most of them hope to obtain.
***
To dig a bit further into this point: some researchers at MIT and Virginia Tech pioneered the idea of applying a basic reproductive parameter (R0) to academia and specifically to biomedical fields.
Their basic assumption is that the R0 in academia should be 1, which means that if academic employment is stable, then over the average professor’s lifetime, he or she should train one PhD student as a replacement. On average, a system like that will supply one new PhD graduate every year for every professor who retires or dies.
Of course, that’s somewhat simplistic. For one thing, in many fields (particularly tech, engineering, economics, etc.), many PhD students will end up finding employment outside of academia. And in some fields (such as computer science), the number of professors has grown dramatically over the decades (as in the case for a field that didn’t exist at one time). In any event, an R0 of 2 or 3 might be fine—it will just mean that an academic field is producing 2 or 3 times as many PhDs as can end up employed in academia.
So, these scholars showed that the R0 in “biomedical fields has increased over time, and we estimate that there is approximately only one tenure-track position in the US for every 6.3 PhD graduates, which means the rest need to get jobs outside academia or stay in lower-paid temporary positions.” In other words, we have been producing 6.3 times as many PhDs in biomedicine as will be able to find jobs in academia (unless universities go on a hiring spree).
That means that the vast majority of PhDs will have to find jobs elsewhere.
Thus, as the New York Times reported in 2016:

Is this still true today?
Well, in 2022, there were 9,386 doctorates granted in biomedical sciences in the United States, while there were 28,953 post-docs supported by NIH funding.
At the same time, the most recent figures I can find from NSF surveys are this:
- In 2019, there were a total of 85,450 professors (of any type) in biological sciences, with 16,200 entry-level assistant professors.
- In 2021, the same numbers had dropped: 84,450 professors total, out of which there were 16,100 assistant professors.
(Source: my own calculations from Table 17 in the 2019 and the 2021 NSF Survey of Doctoral Recipients.)
I cannot find direct figures on how many people left academia (or died) and were replaced. But suffice it to say that when there is a stable number of around 16,000 entry-level professors from year to year, it is mathematically impossible to accommodate upwards of 9,000 new doctorates per year plus nearly 29,000 post-docs who might apply for entry-level jobs in any given year. Many of these people can find jobs in industry, but there are nowhere near enough academic jobs for the people who want them.
In some sense, an imbalance like this is fine, as long as people are well-informed about their prospects, and aren’t being subsidized to make bad decisions.
In acting and music, there are many more aspiring people than jobs as well. But at least we don’t publicly subsidize those people in their mid-30s to spend several years pursuing an acting or music career that will likely never happen.
Another unfortunate result is the continued escalation of credentialism. One former editor of Science told me that in today’s environment, it’s hard to hire a mere PhD as an entry-level professor, because they’re up against people with 5+ years of postdoc experience and many more publications to their name.
That is, entry-level professors are now being held to a standard that likely would have gotten them tenure in prior decades. Where does this escalation stop? Will some people have to wait until age 45 or 50 to get their first tenure-track job in biomedical academia?
Painful Choices
The academic biomedical system needs to make some painful choices. Some 20 years ago, the system overstaffed and overbuilt during the NIH “doubling.” We’re still dealing with the ramifications of that, and the system-wide incentive is to hire tons of low-paid trainees to do most of the lab work so as to churn out more publications (even if many of those trainees have no real future in academia).
This is a destructive pattern. As Alberts, Kirschner, Tilghman, and Varmus wrote in 2014:
There is no more worrisome consequence of the hypercompetitive culture of biomedical science than the pall it is casting on early careers of graduate students, postdoctoral fellows, and young investigators. A recent study commissioned by NIH Director Francis Collins documented the rapid growth in the number of biomedical PhDs and postdoctoral fellows trained in the United States, driven most recently by the doubling of the NIH budget that ended a decade ago. As those trainees complete their studies, they have come face to face with slowdowns or contractions in the employment sectors—academia, government, and the pharmaceutical and biotech industries—that could and should benefit from their long years of training. This has led to an extended occupancy of training positions, coupled to greatly increased expectations from prospective employers for prior productivity.
The NIH is not doing graduate students or post-docs any favors by continuing to subsidize this system in any form. People can end up being strung along for a decade or more, only to finally realize in their late 30s or even early 40s that they won’t get a biomedical professorship after all.
For many of those people, it would have been far better (even if painful at the time) if 10 years earlier, someone had redirected them into industry, consulting, or another career altogether. Better to start over at age 25 than at age 35 or 40.
Indeed, I suspect that even people who might publicly disagree with this essay would secretly agree with me. For example, a policy leader at a well-known scientific organization once told me, “I can never say this publicly, but we were probably stronger 40 years ago when there were many fewer people in the field, and there was less cutthroat competition for grants.”
Policy people can’t say that kind of thing publicly, because their whole mission is to argue, year in and year out, for why their own particular organization/issue/field/disease is so crucially important that it should be more well-funded and employ more people than today. Perpetual growth is their main policy goal. But most people agree, even if silently, that hypercompetition is counterproductive.
Conclusion
In short, when Congress takes up NIH reauthorization in the future, it should consider the following reforms that would help improve both employment and outcomes in biomedical science:
- Mandate that post-docs be paid at least 2.5x (preferably 3x) the median rent for a one-bedroom apartment within 30 minutes of the university in question.
- Mandate that NIH transition to a system in which NIH dollars pay for post-docs only through direct grants (such as F32 or K99), rather than as personnel on another principal investigator’s grant (R01 or otherwise). Many experts have recommended this idea since at least the 1990s, and it would give the NIH more direct oversight over how many post-docs are being funded, at what salary, and over what time frame.
- Mandate that NIH create a plan to reduce the overall number of publicly-funded post-docs over time, and instead work with universities to create a permanent set of staff scientist jobs so as to provide more stable career tracks and salaries for highly-trained PhDs who don’t obtain tenure-track professor positions.
- Mandate that NIH stop paying altogether for anyone to be a post-doc if they are more than 2 years out of a PhD. Such a top-down mandate would be the only way to overcome the collective problem of ever-increasing over-credentialism for academic jobs. It simply shouldn’t be possible for a university to demand 5+ years of post-doc experience for an entry-level professor job. (Indeed, one person who read this column ahead of time suggested that the NIH shouldn’t pay for post-docs at all! But I’ll leave that for another day.)
- Mandate that any university or academic medical center with at least 5 NIH-funded graduate students or post-docs report publicly on the employment outcomes for the last 20 years of the students or post-docs at that institution. This would give graduate students and post-docs much better information on which to base their career decisions.